What Is Revenue Cycle Management in Healthcare?

Collecting more of the billions left on the table means understanding revenue cycle management
This post was published July 12, 2018, and last updated April 8, 2026.
“A billion here, a billion there, and pretty soon you’re talking real money.” That famous, though likely misattributed, quote from US Senator Everett Dirksen.1 Today, it’s become the theme of revenue cycle management in medical billing.
What is revenue cycle management?
A common definition of revenue cycle management (RCM) in healthcare is all the administrative and clinical functions that contribute to the capture, management, and collection of patient service revenue.
The RCM process begins as soon as patients make appointments for your services and continues until you receive full payment from both insurers and patients. A true RCM solution unifies the key components of practice management, electronic health records, and claims processing. It creates an efficient workflow that helps you collect revenue while enhancing the patient experience.
What are the major revenue cycle management challenges for medical practices?
In the United States, revenue cycle management in medical billing requires considerable expertise, attention, and perseverance to navigate. Many practices fail to recognize the importance of revenue cycle management in healthcare, relying instead on disparate systems and disjointed processes that can sometimes result in payments getting delayed or denied.
Revenue can seep from countless cracks in the system, including inadequate monitoring of underpayments and denials, fumbles in patient collections, errors in insurance credentialing and policy coverage, services not billed, clunky hardware and software, and insufficient staffing and training in billing. Other common causes of lost revenue include:
- Coding inaccuracy: Documentation gaps or incorrect CPT/ICD-10 coding that can trigger immediate denials.
- Compliance and audit risk: Failing to adapt to shifting federal regulations and payer-specific policies.
- Credentialing and enrollment: Lapsed or improper provider filings that can make services unbillable.
- Patient financial responsibility: The patient-as-payer shift, where high-deductible plans can lead to increased bad debt.
- Data analytics: Operating without visibility into key performance indicators (KPIs), like days in AR or net collection rates.
Why is revenue cycle management important in healthcare?
A significant cash flow loss can seriously impact a practice’s overall success. And even before the COVID-19 pandemic, billing errors and rejected claims were costing providers billions of dollars per year. Going forward, effective healthcare revenue cycle management could become even more critical.
In 2022, the credit agencies announced sweeping changes to how they would report medical debt, omitting most existing debt and delaying the reporting of new collection activity. The Consumer Financial Protection Bureau estimated that 43 million credit reports showed roughly $88 billion in medical bills.2 The changes are designed to help consumers retain access to credit, but they may also reduce creditors’ leverage to collect medical debt.
In 2021, the White House issued a new rule under the No Surprises Act to limit patients’ out-of-pocket costs. It provided that health insurers and medical providers settle their differences through a new arbitration system when they couldn’t agree on charges.3
Grasp the revenue cycle management process in medical billing
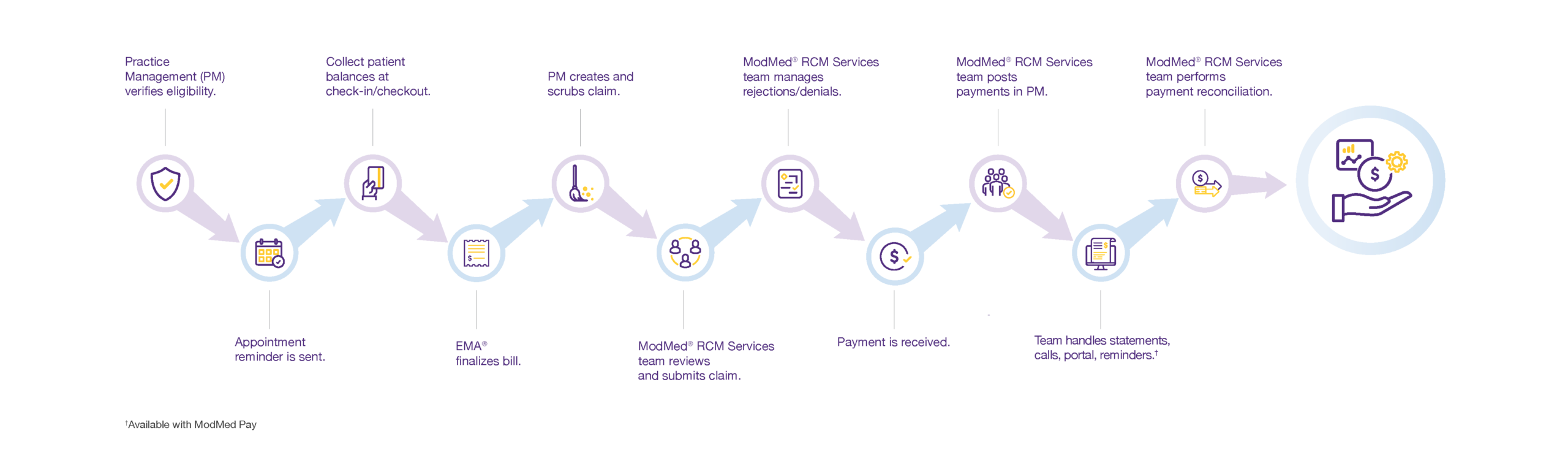
Understanding revenue cycle management, which involves much more than just billing, means understanding the people, processes, and technologies required to increase reimbursements by insurers and payments by patients. Here are the major steps of an RCM service.
Front end: Preservice and patient intake
The front end is the foundation. Errors made here — such as incorrect insurance data — account for the vast majority of claim denials later in the process.
- Eligibility verification. Before patient appointments, the practice management system automatically checks eligibility to avoid problems with reimbursement.
- Patient check-in. Upon arrival, patients check themselves in through a patient portal, their own smartphones, or a kiosk in your lobby.
- Collection. Patient balances are collected at check-in (and checkout).
Mid-cycle: Clinical documentation and coding
This stage bridges the gap between the exam room and the billing office. It focuses on transforming clinical encounters into billable data.
- Billing. During documentation, an integrated electronic health records system creates a bill and suggests codes and modifiers for services.
- Claim creation. The practice management system creates and scrubs claims for accuracy.
Back end: Claims management and collections
The back end starts once the claim is submitted. It’s focused on following the money, resolving disputes, and closing the books.
- Claim submission. Before sending claims, the billing team reviews them for accuracy, then releases them to the clearinghouse.
- Claim rejection. If the clearinghouse rejects a claim, it is returned to the RCM team for correction and resubmission for payment.
- Payment receipt. Insurance payments are transferred to your bank account and posted to patient accounts in the practice management system.
- Patient payments. To help collect patient balances, the system provides detailed statements, inbound call handling and a payment portal.
- Posting. The billing team makes sure that all payments are posted in the practice management system.
- Account reconciliation. The RCM team reviews accounts to confirm that everything adds up, comparing the claims sent with the payments received.
How are practices tying together the revenue cycle?
Using an RCM solution that works seamlessly with your EHR can help eliminate the silos that typically exist between clinical care and billing. For example, using a specialty-specific EHR like EMA® allows clinicians to document exams using structured data. Because the system understands the clinical context, it auto-suggests relevant ICD-10 and CPT codes, which can reduce the manual effort required for claims creation. And automating the flow of data from the exam room to the billing office can help speed up reimbursements.
Our ModMed® RCM Services team handles all the steps listed above for revenue cycle management. Working with our integrated Practice Management and EMA EHR system, we can help your office put the right processes in place to gain vital transparency and run more smoothly, so you can focus on what matters most — patient care. Reach out for a complimentary cash flow analysis to identify opportunities.
Discover how ModMed RCM Services can support your bottom line.
References
1 Amdur, Eli. “A Billion Here, a Billion There, Pretty Soon …” Forbes. April 2, 2021.
2 Andriotis, AnnaMaria. “Most Medical Debts to Be Removed From Consumers’ Credit Reports.” The Wall Street Journal. March 18, 2022.
3 Armour, Stephanie. “Medical Cost Disputes to Be Settled by Arbitrator.” The Wall Street Journal. September 30, 2021.
This blog is intended for informational purposes only and does not constitute legal or medical advice. Please consult with your legal counsel and other qualified advisors to ensure compliance with applicable laws, regulations, and standards.







