
EMA® by Modernizing Medicine
An Ophthalmology EHR System
EMA® by Modernizing Medicine
An Ophthalmology EHR System
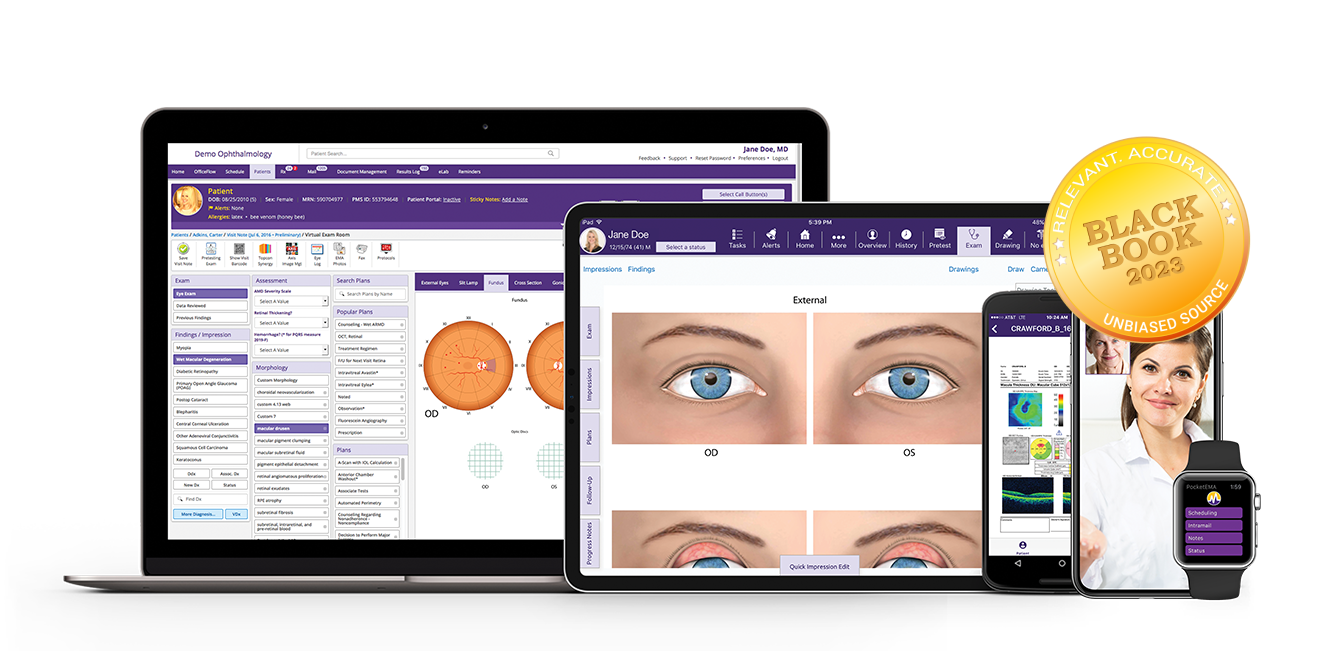
Combining the best that cloud EHR healthcare systems have to offer with the efficiency of specialty-specific software is only part of what makes EMA® the #1 ophthalmology EHR¹ available.
- Subspecialties include: cataract & refractive, glaucoma, retina, oculoplastics and pediatrics
- Easy touch-based ophthalmic EHR solution
- Automated notes and bills
- Built-in ICD-10 ophthalmology codes
- Better overall patient experiences
- MIPS functionality
- Award-winning* User Experience (UX)
¹2023 Black Book Market Research.
*By SaaS Awards and UX Design Awards
Journey Through A Modern Practice
Journey Through A Modern Practice
Right out of the box, our ophthalmology EHR software provides you with over:
Chief complaints
Diagnoses with ICD-10 codes
Treatment plans and procedures
Here's What Your Peers Are Saying

Maria Ruttig, Practice Administrator, Eye M.D. of Niceville
“From my experience, the billing and coding capability is one of the biggest advantages. The ophthalmology EHR system documents everything based upon your input and suggests the right code based upon what you have documented.”

Christine Sykora, Practice Administrator, Advanced Eye Care, SC
“We’re happy with the efficiency we’ve created with EMA. We used to see 650 patients a month on paper and now see over 900 a month with fewer providers and shorter hours. EMA has also been a contributing factor to the 26% increase in revenue we’ve experienced over the last five years.”

Alan R. Malouf, MD, PA
“The ophthalmology EHR training and education we received were so thorough that we were able to continue with our existing patient flow and did not need to decrease our productivity during implementation. If we do need support, the Modernizing Medicine team is always responsive.”
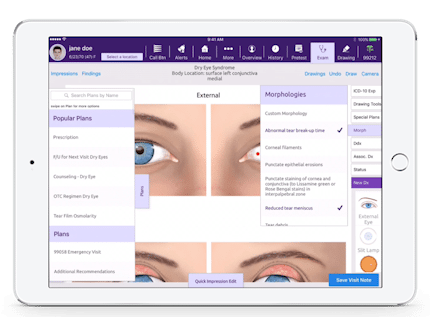
No More Adapting to Your EHR—EMA Adapts to You
Containing subspecialty workflows and clinical knowledge, our ophthalmology EHR provides what you need, when you need it. EMA’s adaptive learning engine recognizes your preferred methods, suggests your top diagnoses and treatments and even anticipates your next move. With a top-rated ophthalmology electronic health records system tailored specifically to your style of practice, you can work faster, without interruption, and with a virtual medical assistant by your side that thinks just like you do!
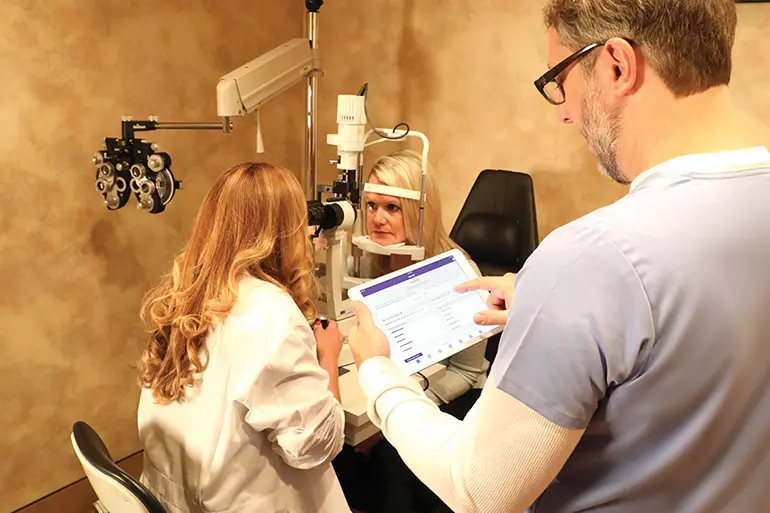
Ophthalmology Practice Management Unhindered
Our #1 ophthalmology EHR is built for iPad use, freeing you up to move around the room and interact with patients instead of typing at a computer. Simply tap the screen to quickly document or show patients key information. All the while, your scribe can work in tandem with you from a desktop computer. At the end of the exam, our ophthalmology electronic medical records system automatically generates a written note and bill, suggesting CPT, ICD-10 and modifier codes for you based on your EMA data. Before the patient even leaves the room, your documentation can be done!
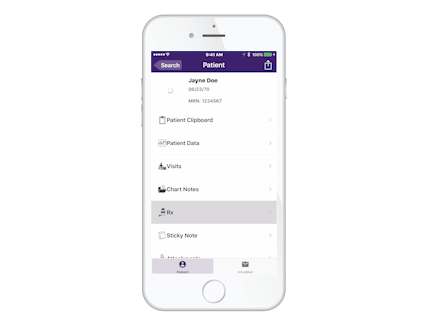
Access Records Remotely
Since EMA is cloud-based, you don’t have to leave your records behind when you leave your office. With PocketEMA™, our ophthalmology electronic medical records app for your smartphone, you can connect to EMA from almost anywhere and check patient charts easily. In most states, you can even ePrescribe. In the office, the PocketEMA Apple Watch app helps make busy days easier by putting your schedule, chart notes, messages and more right on your wrist. Plus, a cloud-based ophthalmology EHR system means you can log in from virtually any iPad or computer—no need to buy, set up or maintain expensive onsite server equipment.
Superior Healthcare Technology Empowers Superior Care
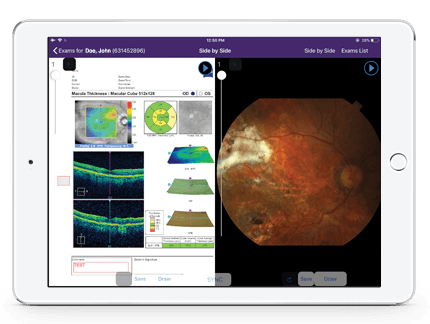
Access Diagnostic Images Right From the Patient’s Chart
Access, review, annotate and share patients’ diagnostic images with the touch of a button from the same system you use to document their visit. Our Image Management system integrates with EMA, automatically uploading images from your connected diagnostic imaging devices.
You can easily review DICOM images from current or historical exams, compare images side by side to assess progression, or sync OCT slices to review dynamic sequences. Whether you’re using the iPad or web version, you’ll have images to help support your diagnostic findings right at your fingertips.
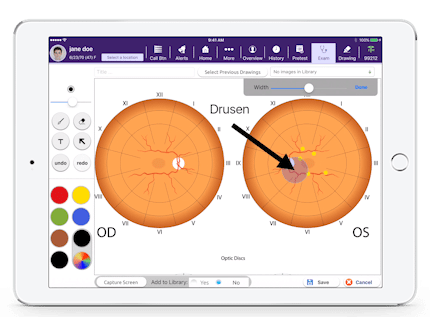
Illustrate Freely With the Drawing Board
Using your finger or an Apple Pencil, you can draw freehand on photos or eye diagrams, and your drawings will be automatically added to the appropriate parts of the patient record. Alternatively, choose from a library of prepopulated drawings or pull forward your previous drawing for the patient, edit it and save it to the current visit note. It’s just another way our leading EHR technology is Modernizing Medicine and shaping the future of ophthalmology software.
Manage Your Optical Inventory
Run your dispensary efficiently and effectively with this intuitive optical inventory solution that interfaces with our ophthalmology EHR. FlexSys combines optical sales, insurance processing of optical goods and reporting in one cutting-edge platform.
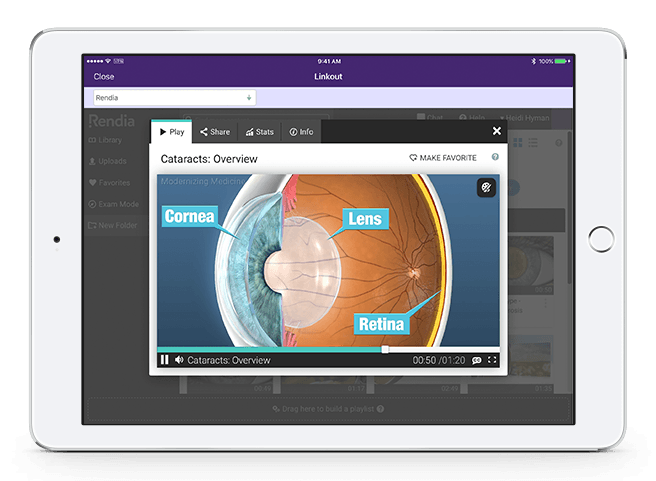
Educate Patients Easily
Rendia is educational software that blends stunning clinical artwork with interactive technology to help medical professionals and patients understand each other better.
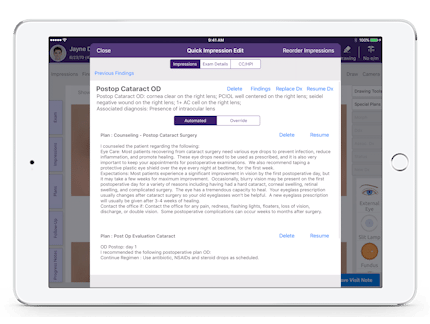
Document Instantly With Protocols
To make the best ophthalmology EHR even better, we’ve created a way for you to document and code an entire visit with just a few taps. Our Protocols feature lets you create master visits for common conditions, procedures or post-op visits, then apply this information to any exam effortlessly. In a few clicks, you can record comprehensive patient, procedure, diagnosis and treatment data, and our ophthalmology EHR will generate a note and bill just as it does for a regular visit.
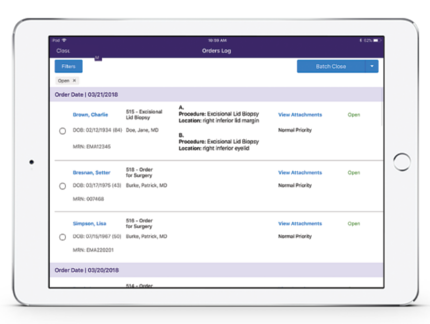
Stop the Surgical Orders Paper Trail
Easily manage all procedure and surgical orders generated by providers and staff in one place with EMA’s orders log. You can add due dates and schedule dates, upload attachments such as prior authorizations, and create and assign tasks to better manage personnel. Plus, keep required documents organized and fax directly from the orders log.
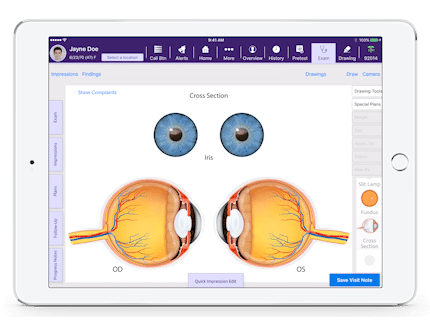
Capture Data Visually With the Interactive Anatomical Atlas™
Taking ophthalmic illustrations to the next level, the Interactive Anatomical Atlas lets you zoom in and peel back its 3D layers to view the fundus, slit lamp, eye cross section and more. It’s an ideal tool for educating patients and, with anatomical locations preloaded, it can even suggest an ICD-10 code automatically when you tap on the touchscreen display.
A Smarter Kind of Data for Ophthalmology
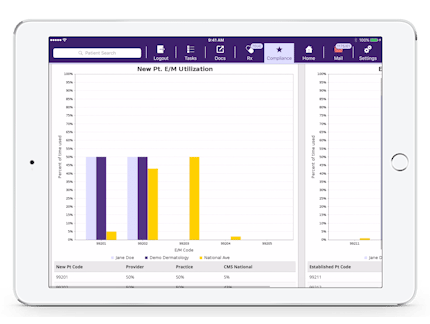
Don’t Just Capture Information; Leverage It to Improve Outcomes
While other ophthalmology software gathers data as free text, EMA primarily collects structured data, so the system can understand what information means and how to harness it. This enables EMA to automate time-consuming tasks like coding as well as run powerful analytical studies. For instance, you can benchmark your E&M and eye code utilization against other providers in your practice and against CMS Medicare Part B utilization data. See what the best ophthalmology EHR looks like with a free demo.
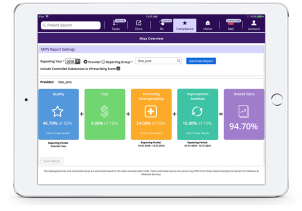
Be Better Prepared for MIPS and MACRA
Now that Meaningful Use (MU) and PQRS have become part of MIPS, CMS is paying ophthalmologists on a curve. To maximize your chance of success under MIPS, it’s vital to know where you stand before the reporting deadline arrives, so you can adjust as needed. With powerful benchmarking tools, our built-in MIPS solution can help you do just that.
Modernizing Medicine®’s 2015 Edition Certified EMA ophthalmology EHR can not only compute your MIPS measures automatically within the flow of the exam, but also show you how we believe you’re performing compared to your peers. This can help you stay on track for MIPS success while dedicating more time to your patients. Learn more about MIPS and MACRA here.
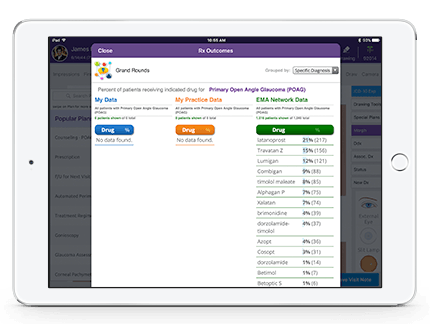
Practice Evidence-Based Medicine
Easily visualize patient progress over time with EMA Outcomes, part of our advanced ophthalmology EHR system. Plus, view top treatments for specific diseases by using Grand Rounds to learn from a nationwide community of your ophthalmology colleagues. By drawing on clinical evidence, these EMA medical features can enhance your diagnostic and treatment power to improve outcomes and quality of care.
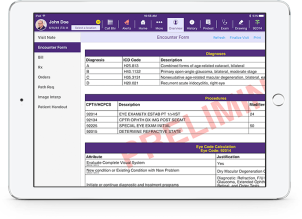
Make Ophthalmology ICD-10 Easy
Many ophthalmology EHR systems risk inaccurate coding and claim denials by forcing you to use ICD-10 codebooks, lookups or translation tools. EMA, on the other hand, uses Modernizing Medicine’s innovative technology to suggest specific ICD-10 codes automatically. Not only does this save time, but also our clients frequently discover that they improve their ophthalmology billing accuracy.
Integrated Ophthalmology Inventory Management
By using an integrated Inventory Management system, it can help improve tracking of intravitreal injectables and products such as drops, while helping to decrease costs by mitigating lost inventory. See more here.

Responsive, Personalized Support
Through onboarding and beyond, Modernizing Medicine offers award-winning training and support from dedicated team members, working to ensure your ophthalmology practice management is smooth from the get-go.
What Is the Top-Ranking Ophthalmology EHR System?
Black Book™ Research, an unbiased research organization, has conducted their yearly comprehensive survey of ophthalmologists and healthcare leaders nationwide. For the 7th year in a row, their choice for the #1 ophthalmology EHR system is EMA, Modernizing Medicine’s Cloud, Mobile, Touch solution for ophthalmology practices. It’s a testament to EMA’s effectiveness and rapidly growing impact on the ophthalmology EHR market.
Ophthalmology EHR Software: Free Download or Demo?
Many vendors offer a free EHR software download as a try-before-you-buy incentive. Sounds fine on paper, but what can you really expect from a free download? Probably not much. It might provide a vague sense of features and functionality but zero insight into how the software can help empower your practice.
Modernizing Medicine doesn’t offer free downloads because our ophthalmology software can be customized to fit different practice workflows. What we do provide are free personalized demos that quickly and clearly show how we can help you leverage our ophthalmology EHR. So, skip the free download and schedule your demo today!
Real-World Results
minutes per patient saved compared to his old EHR– Dr. Gilbert Wong
eye care providers nationwide use EMA
eye care visits have been documented with EMA
Ophthalmology Resources
Please choose from the menu below
Videos
Webinars
Success Stories
Educational Guides
Blog
Events









